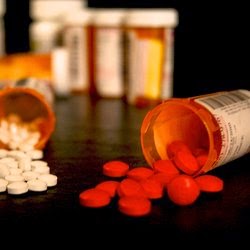
So here's a quick rundown on Day 1 of my first cycle of chemo.
All things considered, it was actually pretty easy. The only real side effects so far are a bit of a headache and the weird thing where my throat freaks out if I drink anything really cold. So, no more iced drinks for me for awhile.
The pump for the forty-six hour 5-FU infusion has been running since 2:00 pm, and it's proven to be okay to manage. It runs solely on batteries, so I don't have to worry about plugging it in, and the pump and bag of drugs all fit in the fanny pack that came with it. There's only one tube running up to the chest port, so it's all reasonably convenient. The only real downside is that it's heavy, so having it hang off your waist the whole time gets old. I find I'm taking it off and setting in on a table or window sill if I'm going to be in one place for awhile.
So basically, Cycle 1, Day 1 of chemo has been pretty much a cake walk. Of course, this round didn't include Avastin -- Avastin slows healing so they need me to be further past the port installation before starting me on that -- and I'm told Avastin has a pretty big wallop. Also, chemo is a cumulative treatment, so things are supposed to get worse as you go along. One of my cancer informants told me that her first cycle didn't hit her until Day 3, so I'm not out of the woods yet.
But still, I'll take the easy day today and we'll just wait and see what happens tomorrow.
This is my blog about my cancer ("my cancer," like it's a pet or a hobby). I'm starting it because I'm fairly lazy and repeating the same stories over and over as friends and family ask about the latest development seems really inefficient. This also gives everyone access to the same source material, thus minimizing the "telephone" problem. We'll see if it works and how long I bother to keep it up...
Wednesday, July 30, 2014
Chemotherapy is Unamerican
I've been fortunate enough to have a few opportunities to travel internationally and it's true: Americans do get a fair amount of grief over their love affair with ice. People just don't get why we want ice cubes floating in all our beverages.
It's because ice is awesome. Chewing ice is awesome. Everything about ice is awesome. There's nothing better than a lovely summer beverage filled with crushed ice.
Well, unless and until you're getting treated with oxaliplatin. Apparently, one of the side effects of oxaliplatin is increased sensitivity to cold. So much so that drinking cold beverages can cause you to feel like you're throat is constricting and you can no longer breath. So, for the remainder of my chemotherapy regimen I'm supposed to avoid iced beverages and only drink things that are room temperature or warmer.
It's downright unamerican.
It's because ice is awesome. Chewing ice is awesome. Everything about ice is awesome. There's nothing better than a lovely summer beverage filled with crushed ice.
Well, unless and until you're getting treated with oxaliplatin. Apparently, one of the side effects of oxaliplatin is increased sensitivity to cold. So much so that drinking cold beverages can cause you to feel like you're throat is constricting and you can no longer breath. So, for the remainder of my chemotherapy regimen I'm supposed to avoid iced beverages and only drink things that are room temperature or warmer.
It's downright unamerican.
The Inaugural Chemotherapy Live Blog
So this will either turn out to be a really great idea or a
really stupid one, but assuming I don't get kicked off the GHC visitor network I figured
I’d try to live blog my first chemotherapy session.
Come back throughout the day for updates (assuming I don't start feeling too bad to be typing)...
8:00 am
Sib4 arrives at the condo to keep my company for the day. She left her
house at 6:45, so a fairly ugly commute in. It does make me glad I can walk three blocks to my chemo session rather than having to drive across the state the way some people must.
8:15 am
On the recommendation of some co-workers we elected to try the Volunteer Park Cafe for breakfast. I had a lovely stuffed french toast with caramelized bananas and Sib4 opted for the granola with yogurt and apricots. I can definitely recommend the french toast. The coffee was kind of weird, though.
9:10 am
My chest port gets its inaugural use, though for the purposes of drawing blood out rather than putting chemo in. All things considered, it was pretty straightforward. The nurse grabs the port, has you inhale and then exhale, and jabs the needle into the port during the exhale. It'll stay there for the next three days for the chemo infusion. The blood draw takes five minutes, and then we cross the hall to wait for my 10:10 appointment with the oncologist.
9:20 am to 9:45 am
Waiting...
9:45 am
The nurse takes me back to the exam room to wait. On the way in, she weighs me. My official pre-chemo starting weight is 218 pounds. We'll see what it is in a few months.
9:55 am
The oncologist comes in for a brief chat. Mostly she's there to answer any questions I or Sib4 might have. I have two. First, how was the chest scan? Happily, while I have "nodules" in my lungs, everyone does and they aren't necessarily a sign of cancer (but will be watched). Second, does she think I'll make Book of Mormon? On that issue, she's hesitant to comment. But I'm cleared to proceed with chemo, so we'll see.
10:05 am to 10:20 am
Waiting...
9:45 am
The nurse takes me back to the exam room to wait. On the way in, she weighs me. My official pre-chemo starting weight is 218 pounds. We'll see what it is in a few months.
9:55 am
The oncologist comes in for a brief chat. Mostly she's there to answer any questions I or Sib4 might have. I have two. First, how was the chest scan? Happily, while I have "nodules" in my lungs, everyone does and they aren't necessarily a sign of cancer (but will be watched). Second, does she think I'll make Book of Mormon? On that issue, she's hesitant to comment. But I'm cleared to proceed with chemo, so we'll see.
10:05 am to 10:20 am
Waiting...
10:20 am
The nurse takes me back to my designated infusion space. Now she's got to order up my designated drug cocktail (I was given a handout at my first appointment explaining why chemo "is not like a milkshake"). Sib4 also got a tour of the kitchenette, and the beverage options that I have available. Most important, we learn that once the chemo starts I'll be here for two-and-a-half hours. And, of course, I'll go home with a machine set to deliver a second infusion over the next forty-eight hours.
11:00 am
I've been given the two anti-nausea medications, one of which is going to make my blood sugar go through the roof, but still waiting for the chemo meds to show up.
11:15 am
The chemo has arrived. And here we go...
12:00 pm
So for the last forty-five minutes the nurse educator has been going over the drugs I'm getting, how to respond to the various side effects, and providing an orientation to the treatment regimen. In short, I'll repeat today's experience three more times -- Avastin being added to the drug cocktail in session 3 -- and then they'll take a scan to see if there's been any impact.
Forty-five minutes in and I'm not really feeling anything from the chemo yet.
12:15 pm
Hey! Chemo comes with lunch. In this case, a nice grilled chicken, corn, green beans and watermelon. Non-diabetics probably got chips or crackers or something, too, as I get a scoop of guacamole but nothing, really, to put it on. Non-diabetics also get orange slices in place of watermelon (which we know because the nurse came in and traded out my original oranges). Sib4, unfortunately, has to starve, but we'll probably go find second lunch after the chemo experience is over.
Still no real sense of any side effects yet. Fingers crossed...
12:31 pm
OK, my first side effect: headache. We'll see if the nurse will bring me some Tylenol. (I normally use Excedrin, but aspirin is now on the do not take list.)
12:45 pm
The nurse gives me the rundown on how to use the home infusion pump for the next phase of this cycle. Most happily, she agrees to train me on how to remove and flush the tubing from my chest port so I don't have to come back to GHC to have someone else remove it. I can just take it out myself and then drop the pump off when convenient. Sweet!
1:00 pm
It's time to test the fire alarms. Go figure. The nurses all leave to run through they're emergency planning, but at least they don't make me drag my IV pole downstairs and outside. I get to sit in my chair and continue the infusion -- which is enough to make me figure that this is just a test.
1:16 pm
The chemo bags are empty, so phase 1 of this cycle is done. Now the nurse just has to get me hooked up to the pump and the 5-FU and I should be good to go. But she's got another patient to deal with first.
2:13 pm
Done and done. Home pump is hooked up and in my free fanny pack, and we're good to go. Off to get some anti-nausea pills and then we're outta here. If chemo continues like this -- unlikely, no doubt -- I'm golden.
Tuesday, July 29, 2014
Countdown to Chemotherapy
I'm having a failure of imagination.
Tomorrow is my first chemotherapy infusion and I've reached the point where I'm realizing I just cannot begin to imagine what it's going to be like. I've read all the "what to expect" manuals. I've talked to all the people I know who've been dealing with chemotherapy themselves. I can do the rundown on side effects in my head. What I can't do though is project myself into the future to create any sort of idea of what the experience will be like. Or rather, all I can project into the future is my current self and my current self isn't wrestling with any of the side effects of chemotherapy. My current self feels pretty good, and so my assumption is that the same will be true tomorrow when they're dripping weirdness into my new chest port.
How could it be otherwise? How could I not be in a condition to go back to work on Thursday or, more important, use my ticket to Book of Mormon on Thursday night.* What does, say, a low blood cell count, or whatever, feel like? How bad can this be, really?
Truly, I can't even begin to imagine. It must be the pants.
* I bought the ticket to Book of Mormon long before the cancer diagnosis, and they're now very hard to get and impossible to exchange. I'm really hoping the chemo infusion won't prevent me from going to my scheduled show on Thursday.
Tomorrow is my first chemotherapy infusion and I've reached the point where I'm realizing I just cannot begin to imagine what it's going to be like. I've read all the "what to expect" manuals. I've talked to all the people I know who've been dealing with chemotherapy themselves. I can do the rundown on side effects in my head. What I can't do though is project myself into the future to create any sort of idea of what the experience will be like. Or rather, all I can project into the future is my current self and my current self isn't wrestling with any of the side effects of chemotherapy. My current self feels pretty good, and so my assumption is that the same will be true tomorrow when they're dripping weirdness into my new chest port.
How could it be otherwise? How could I not be in a condition to go back to work on Thursday or, more important, use my ticket to Book of Mormon on Thursday night.* What does, say, a low blood cell count, or whatever, feel like? How bad can this be, really?
Truly, I can't even begin to imagine. It must be the pants.
* I bought the ticket to Book of Mormon long before the cancer diagnosis, and they're now very hard to get and impossible to exchange. I'm really hoping the chemo infusion won't prevent me from going to my scheduled show on Thursday.
Sunday, July 27, 2014
John's Instant Amnesia
I discovered this recipe today, and found it to be incredibly useful for forgetting about cancer, chest ports, chemotherapy and whatever other crap life may have dropped in your lap.
For those without easy access to all of the ingredients, the outcome could presumably be just as successful with a few substitutions to account for one's personal situation and taste.
Instant Amnesia
1 Convertible with a passable car stereo
1 CD, mix tape, iPod or flash drive (as appropriate) loaded with your favorite songs
1 Lovely sunny day
1 National Park of your choice
Mix all ingredients together. Serves 1-6, depending on the convertible.
For those without easy access to all of the ingredients, the outcome could presumably be just as successful with a few substitutions to account for one's personal situation and taste.
Instant Amnesia
1 Convertible with a passable car stereo
1 CD, mix tape, iPod or flash drive (as appropriate) loaded with your favorite songs
1 Lovely sunny day
1 National Park of your choice
Mix all ingredients together. Serves 1-6, depending on the convertible.
Friday, July 25, 2014
Thursday, July 24, 2014
Second Guesses
I've been a Type I diabetic for a little over twenty-eight years. Long enough that I can't really remember not being a diabetic. Sure, I've got vague recollections of being able to eat sugary foods, or skip a meal without worrying about the impact on my blood sugar, but that's not really the same as knowing what it feels like not to have diabetes.
There are lots of bad things about diabetes -- high blood sugar, low blood sugar, daily injections, etc. -- but the one that actually bugs me the most is the fact that it's always there. You don't get to take a vacation from being diabetic. As a result, everything you feel and experience runs through the diabetic filter: Am I hungry, or is it just low blood sugar? Am I tired, or is it high blood sugar? Am I, fill in the blank, or is it the diabetes?
It gets really old.
And now, joy of joys, I'm finding that cancer provides for a very similar experience. Every ache, pain, twinge, cramp, irritation, discomfort, whatever, now has to run though the cancer filter.
Did I eat a bad meatball or is it the cancer?
Did I step on a rock or has the cancer moved into my bones?
Is it just a headache or do I now have brain cancer as well?
Does the car next to me have a problem with its catalytic converter or has the cancer taken root in my lungs?
Yes, it's a little nuts, but this is how my brain works. And I'm sure lots of people dealing with chronic health issues can relate. For those of you fortunate enough not to have had the experience, just know that the compulsion to constantly second guess every experience of your body is exhausting. At least it is for me.
I much preferred not wondering if every new twinge is the one that's going to kill me.
There are lots of bad things about diabetes -- high blood sugar, low blood sugar, daily injections, etc. -- but the one that actually bugs me the most is the fact that it's always there. You don't get to take a vacation from being diabetic. As a result, everything you feel and experience runs through the diabetic filter: Am I hungry, or is it just low blood sugar? Am I tired, or is it high blood sugar? Am I, fill in the blank, or is it the diabetes?
It gets really old.
And now, joy of joys, I'm finding that cancer provides for a very similar experience. Every ache, pain, twinge, cramp, irritation, discomfort, whatever, now has to run though the cancer filter.
Did I eat a bad meatball or is it the cancer?
Did I step on a rock or has the cancer moved into my bones?
Is it just a headache or do I now have brain cancer as well?
Does the car next to me have a problem with its catalytic converter or has the cancer taken root in my lungs?
Yes, it's a little nuts, but this is how my brain works. And I'm sure lots of people dealing with chronic health issues can relate. For those of you fortunate enough not to have had the experience, just know that the compulsion to constantly second guess every experience of your body is exhausting. At least it is for me.
I much preferred not wondering if every new twinge is the one that's going to kill me.
Wednesday, July 23, 2014
Port Report
First and most obviously, I didn't die or fall into a coma. Yay for me!
Second, Voila! Doctors now have easy access to the blood flowing into my heart via a chest port. You can see the device in this picture of the x-ray they were using that I took with my phone when the procedure was finished. The port is the triangle shape on the left, and then the little tube runs up from the port to about my collar bone, makes the turn and drops into whatever the big vein up there is, and then runs inside the vein down toward my heart.
Third, I have no idea what those little black dots are near the bottom of the x-ray, but they're kind of freaking me out. They don't really look like the sort of thing that belongs there, but maybe they're perfectly normal. What do I know? I assume I'll find out next week when I meet with my oncologist before my first round of chemo. They took a CT scan of my chest last week and I'm figuring a report on the results will be part of that appointment's agenda.
The procedure to install the port was actually pretty straightforward, at least from where I was sitting. This time, I was actually awake for the whole thing; awake, but not really engaged. They had my face covered so I couldn't really see anything, and the only thing I felt was when they set the port into position. Someone said, "you'll feel a little pressure," and then I felt this crazed wiggling and pushing on my chest. But it only lasted a few seconds and wasn't a big deal. Aside from that, it was mostly just a matter of laying there.
Looking at it from the outside later, the most obvious indications that something happened are the incision above the port that they used to place it and then a second, smaller incision up where the tube makes the turn that they used to get the tube into the vein. Aside from that, there's not much to see. The port sits below the skin, but you can barely notice it's there. I, on the other hand, am very aware it's there and keep wanting to touch it. I can also sense the tube running up to my collar bone and keep wanting to rub at that, too.
I'm hopeful that over time I'll start to forget that the stuff is there. Of course, there's also a perverse part of me that thinks it would be amusing to go get "Insert chemo here" with a little arrow tattooed next to the port.
But I'll let the incisions heal first, at least.
Update:
As I think more about it, I 'm starting to think those black dots on the x-ray may be the leads from the surgical monitors they had on me. Apologies for any inadvertent panic I might have caused.
Second, Voila! Doctors now have easy access to the blood flowing into my heart via a chest port. You can see the device in this picture of the x-ray they were using that I took with my phone when the procedure was finished. The port is the triangle shape on the left, and then the little tube runs up from the port to about my collar bone, makes the turn and drops into whatever the big vein up there is, and then runs inside the vein down toward my heart.
Third, I have no idea what those little black dots are near the bottom of the x-ray, but they're kind of freaking me out. They don't really look like the sort of thing that belongs there, but maybe they're perfectly normal. What do I know? I assume I'll find out next week when I meet with my oncologist before my first round of chemo. They took a CT scan of my chest last week and I'm figuring a report on the results will be part of that appointment's agenda.
The procedure to install the port was actually pretty straightforward, at least from where I was sitting. This time, I was actually awake for the whole thing; awake, but not really engaged. They had my face covered so I couldn't really see anything, and the only thing I felt was when they set the port into position. Someone said, "you'll feel a little pressure," and then I felt this crazed wiggling and pushing on my chest. But it only lasted a few seconds and wasn't a big deal. Aside from that, it was mostly just a matter of laying there.
Looking at it from the outside later, the most obvious indications that something happened are the incision above the port that they used to place it and then a second, smaller incision up where the tube makes the turn that they used to get the tube into the vein. Aside from that, there's not much to see. The port sits below the skin, but you can barely notice it's there. I, on the other hand, am very aware it's there and keep wanting to touch it. I can also sense the tube running up to my collar bone and keep wanting to rub at that, too.
I'm hopeful that over time I'll start to forget that the stuff is there. Of course, there's also a perverse part of me that thinks it would be amusing to go get "Insert chemo here" with a little arrow tattooed next to the port.
But I'll let the incisions heal first, at least.
Update:
As I think more about it, I 'm starting to think those black dots on the x-ray may be the leads from the surgical monitors they had on me. Apologies for any inadvertent panic I might have caused.
It's Chest Port Day
Today is chest port day.
I am not excited about chest port day.
While I understand the benefits of a chest port, from my perspective there are two major downsides to chest port day.
First, this is pretty much the first big thing that makes the cancer real. It's not a surgery to eliminate a painful problem. It's not a diagnostic event. This is someone filling me with plastic tubing (see, told you) to make the future delivery of chemotherapy easier. The chest port is going to make denial awfully difficult to maintain.
Second, and more important, while my Dad was facing a much different situation than I am, and he was in really terribly shape at the time, the primary cause of death for my Dad was the installation of a chest port. He threw a clot during the procedure and never woke up.
Yeah, not at all excited about chest port day.
And on that happy note, it's time to shut down the computer and walk over to Group Health. Presumably, I'll be back in a few hours to report on the result.
I hope so, anyway.
I am not excited about chest port day.
While I understand the benefits of a chest port, from my perspective there are two major downsides to chest port day.
First, this is pretty much the first big thing that makes the cancer real. It's not a surgery to eliminate a painful problem. It's not a diagnostic event. This is someone filling me with plastic tubing (see, told you) to make the future delivery of chemotherapy easier. The chest port is going to make denial awfully difficult to maintain.
Second, and more important, while my Dad was facing a much different situation than I am, and he was in really terribly shape at the time, the primary cause of death for my Dad was the installation of a chest port. He threw a clot during the procedure and never woke up.
Yeah, not at all excited about chest port day.
And on that happy note, it's time to shut down the computer and walk over to Group Health. Presumably, I'll be back in a few hours to report on the result.
I hope so, anyway.
Twenty Questions Is Nineteen Too Many
You wouldn't think weed would be so hard to find in Washington state, but this is new territory for me.
So Sib4 (whose eighteen-year-old is finding great humor in the whole adventure) has found some folks who operate a website intended to educate potential patients on the ins and outs of medical marijuana vis-a-vis cancer. In retrospect, it’s pretty much the standard alternative treatment shtick: parent is diagnosed with cancer and given weeks to live; someone gives parent weed and, lacking any other options, parent gives it a shot; two days later they’ve climbed out of their bed, a week later they’re out in the garden weeding, and a decade later they’re still alive, kicking and cancer-free.
Lovely. Inspiring. Sign me up.
Signing up starts with a phone consultation. Not a problem, except that the calendar and payment system on their website is buggy at best. The calendar identifies three possible appointments weeks in the future, and the payment seems to charge both my PayPal account and my credit card. (The system really, really wants me to use PayPal, so much so that when I enter my credit card information it uses the info to locate my PayPal account and charge that, too.) Once I’ve scheduled the appointment, the folks are nice enough to email me – well, sort of, they, too, have their own web-based communication system – and tell me they have some earlier openings. Nice, but couldn’t those have been on the calendar? All things considered, I have to count this entire process as strike one.
Sib4 is interested in hearing what these folks have to say, so she decides to join me on the call. The weed advisor guy sets up a conference line, and though there’s some confusion about access, we eventually connect. The guy tells his story and then starts running through the various options for cannabis that might help me. Sadly, in this guy’s opinion neither smoking weed nor ingesting it will help me. I either need “cannabis oil” or -- well, for the record, cannabis suppositories will not be happening so we’ll just stick with the cannabis oil. More problematically, he tells me to avoid the medical marijuana dispensaries that are popping up on every street corner in Seattle, as you “can’t trust” their product. Instead, he will provide an introduction to a cost-effective mail order supplier.
This is the word for word email exchange his referral produces, minus the identifying names:
Advisor Guy:
Hi [me],
It truly was a pleasure speaking with you and [Sib4] today. As mentioned, here are some links per our discussion. Please know at any time if you have any questions, I am more than happy to help out.
I have also cc’d [Supplier Rep] with [Supplier] in this email. She can send directly to you.
[Supplier Rep], we discussed a 3:1 THC:CBD ratio for [me].
Supplier Rep:
Hello [me],
Please let me know what questions you have we would be happy to help in any way we can.
[X]
Me:
Hi [X],
I guess I just need to know how to order, pay, etc., for the oil [Advisor] identified in his email.
Thanks!
[me]
Supplier Rep:
Are you a California patient?
Me:
No, I live in Seattle.
[me]
Supplier Rep:
Ok no problem, as far as receiving payment do you have a Bank of America near you?
Me:
I'm sure I could find one.
[me]
At this point, eleven days pass...
Me:
Hi [X],
It seems like I lost the thread of this conversation, so I'm trying to restart it.
Again, per the recommendation from [Advisor] at [Advisor’s Group], I'm trying to purchase 3:1 THC:CBD cannabis oil to help with my colon cancer. My chemotherapy starts next week and I was hoping to get started with the oil before that happens, but that may not be possible now. In any case, sooner rather than later is good.
I live in Seattle, but [Advisor] says you guys can reliably ship, so I'm hoping that's true. I just need to know how to submit the order, how much it will be, and how to make payment.
Let me know what I need to do or, if you can't help me, let me know that so I can try to pursue some other options.
Thanks much,
[me]
Supplier Rep:
Hi [me],
Yes we can make you a 3:1 ratio oil for you. This oil is $35 a gram.
And now my head explodes.
There’s a long tradition of Hollywood movies based on a premise of drug dealers getting themselves into trouble by using too much of their own product. I always thought they were comedies. Who knew they were documentaries?
Have You Tried Your Cancer Baked?
While there are certainly those that would characterize
medical marijuana as another brand of snake oil, there are a few good(ish, maybe) reasons,
I think, to take it more seriously than hydrogen peroxide, vitamin B17, orgone
accumulators and the like.
First, the arguments in support of medical marijuana come
with much higher production values. The YouTube videos attesting to the
curative values of most natural products are, quite frankly, crap. I’ve skimmed
through forty-five minutes of a poorly recorded radio show running behind an
unchanging photo of a vegetable basket, and seen more out of focus selfies
created by self-identified experts than I care to remember. But check out this
video arguing for the cancer curing powers of marijuana (assuming you have an hour
to burn, that is):
Interesting editing, nice use of archival footage, reasonable-seeming talking heads -- now doesn’t that seem persuasive? And while he’s no Morgan
Freeman, doesn’t Peter Coyote (the guy who played the man with the keys in E.T.
thirty years ago) makes for an awfully convincing narrator? The medical
marijuana folks have clearly learned the lessons of Marshall McLuhan and Mad
Men: PR and packaging matter.
Second, unlike most of the snake oil salespeople, most of
the medical marijuana advocates (at least that I’ve seen) are smart enough not
to argue weed as an all or nothing deal. While Suzanne Sommers wants you to
turn your back on Western medicine and embrace the power of her natural juices
(or whatever the hell it was she was hawking), the weed folks seem willing to
entertain the idea that their product might work in conjunction with, rather than
competition with, with standard therapies. And while it may just be me, I’m far more
inclined to try something that doesn’t require me to leap of the top of the
building in the hope that the napkin I’ve just been handed will, in fact, magically turn
into a parachute.
Third, you can’t really deny the impact of medical marijuana’s
rather large, and unexpectedly effective, political moment. Here in Washington,
medical marijuana’s been legal for a few years, and the drug was legalized for
recreational use in our last election. (Legal sales officially started two
weeks ago.) And while the Feds continue to hold to their crazed belief that the impact
of weed is commensurate with meth, heroin, and the rest of the Schedule I drugs,
eventually they’ll have to realize that when politicians start talking publicly
about their own histories of using and people are seeing DEA agents confronting
little old (Caucasian) ladies in wheelchairs demanding access to marijuana,
that particular front in the drug war is pretty much a lost cause.
Fourth, the doctors I talked to, at least, were open to the
idea that marijuana might be useful. Now granted, they figured that the various
anti-nausea drugs and what not that they could offer would be far more effective
than weed, but at the same time they were willing to acknowledge that you
couldn’t overdose on weed, it couldn’t really do any harm, and significant portions
of their patients were using.
Can’t hurt? Might help? Good enough for me.
But then I tried to get the stuff. Kafka would've had a field day. I, on the other hand, would rather give myself root canal than deal with any of those people again.
Monday, July 21, 2014
Try Not to Slip on the Snake Oil
Like everybody, I'm fully convinced that I'm the center of the universe and, furthermore, that the universe can't possible be done with me yet. Death is for everybody else. I'm supposed to be immortal.
But there's nothing like a bunch of people in lab coats telling you that, no, you are actually going to die -- and probably soon -- to screw with one's confidence in those beliefs.
So I'll admit it. I’m starting to get a little desperate. But that's not necessarily a bad thing as desperation has some interesting effects. If nothing else, it's a very useful tool for opening one’s mind. All sorts of ideas
that under normal circumstances would be dismissed out of hand suddenly start to seem quite plausible.
For example, who knew that so many common household items could cure cancer? Hydrogen peroxide, apple seeds, apricot pits, tumeric, baking soda, distilled water, juiced ginger root, flax seed, grapes, walnuts, mushrooms and coffee (not drunk, but used as an enema) are all cancer cures.
And vitamins! Both vitamin B17 and vitamin D (well, D3 not D2) will cure cancer, though B17 has, of course, been "banned" by the FDA, American Cancer Society and American Medical Association.
Then there's the machines and energy manipulations: bioresonance, electrohomeopathy, the Quantum Xrroid, orgone accumulators, magnets, light boxes, rife frequency generators, and zoetrons, among others.
All this too pedestrian for you? How about cat poop? Apparently there's a parasite in cat poop that cures cancer.
(And then, of course, there's cannabis. But weed deserves it's own post, so we'll come back to that later.)
Perhaps it's just me, but eventually you start to realize that an open mind and an internet connection can be a dangerous combination, and that, to borrow a phrase, it's possible to be so open-minded that your brain leaks out. Snake oil is still snake oil, even when it's supported by a ninety minute YouTube video.
But I do sort of wish everyone could hawk their self-discovered anecdotal cures without slagging on the offerings of traditional medicine. I have zero faith that swigging hydrogen peroxide or chewing apple seeds will cure my cancer, but there's only so many times you can hear that "cancer doesn't kill people, cancer 'treatments' do" before your lizard brain starts telling you to run.
Sunday, July 20, 2014
Side Effects
A few years back I read a piece by Steve Martin in the New
Yorker called “Side Effects.” I’d link to it here but I couldn’t find a copy
not hiding behind a paywall, so I’ll just have to state that it’s worth seeking
out. (It was included in his anthology, Pure Drivel.)
I was thinking about Martin’s essay this weekend, as I
decided it was a good time to read through the packet of information I was
given at my first oncology appointment. The drug information sheets were
particularly striking.
I was given sheets for five different drugs that would be part of my chemo regimen: bevacizumab, dexamethasone, fluorouracil, leucovorin, ondansetron,
oxaliplatin, and prochlorperazine. Included in the information provided
for each drug were the “common” side effects, “less common” side effects, and
the things that, if they occurred, should prompt an immediate call to the
doctor.
So across my five drugs? Fifty-two common side effects,
sixty-four less common side effects, and seventy-nine things that should prompt
an immediate call to the doctor. Of course the numbers drop significantly when
you eliminate the duplicates (39, 54 and 41, respectively), but still.
But it’s not the number of items on the list (alone) that
floored me, it’s what’s on the list. The following makes up the list of
“common” and “less common” side effects, we’ll come back to the things that are
supposed prompt an immediate call to the doctor. And at this point I wish I was Gilbert or
Sullivan or Rodgers or Hammerstein or some such, as this really ought to be set to music:
Dry skin, flaky skin; skin rash, skin reaction, skin irritation, including, but not
limited to, burning, stinging, tingling, redness and/or itching; acne; skin
darkening*; splitting fingernails; brittle hair, thinning hair, hair loss
and/or increased body hair. (So you’re telling me chemo is like bizarro world
puberty? Joy.)
Dry mouth, mouth sores, trouble swallowing, trouble talking, jaw
tightness, odd feelings in your tongue and/or a metal taste in your mouth.
(It’s probably inappropriate to suggest that the metal taste might be a
function of the gun barrel.)
Loss of appetite, increased appetite, increased thirst; weight
loss, weight gain, water retention; abnormal fat distribution. (Sadly, there
are no photographs to document “abnormal fat distribution.” This I'd like to see.)
Constipation, diarrhea; frequent urination, trouble urinating
and/or pink or brown urine; stomach ulcers, holes in your intestine; nausea,
vomiting, stomach cramps and stomach upset. (Well, you can hardly blame the
stomach for being upset with all that going on.)
High blood pressure, low blood pressure; bruising; blood clots,
nose bleeds and/or serious bleeding; high blood sugar; low blood cell counts.
(Although maybe the cells are just giving up and running away.)
Changed vision, blurred vision, cataracts, glaucoma and/or watery
eyes. (Of course, those might just be tears from all these insane side
effects.)
Irregular heartbeat, heart attack, heart failure; slowed healing
and increased risk of infection; dizziness, headache, seizures, stroke; decline
in liver function, decline of kidney function, bone loss. (Can we just go back to
bizarro puberty?)
Scarring of the lungs, tightness in the chest and throat, trouble
breathing and/or feeling like you’re not breathing even though you are. (OK, now
you’re just yanking my chain. How are you supposed to distinguish between the
imaginary breathing problems and the actual breathing problems?)
Muscle spasms, tremors; weakness, tiredness, weakness,
restlessness, nervousness, inability to sleep and mood swings. (Yeah, my mood’s
swinging already.)
Pain. (Sigh.)
And if that weren’t bad
enough, we still have the items that are considered serious enough to require
an immediate call to the health care team: abdominal pain, abnormal bleeding
(versus normal bleeding?), allergic reaction, back pain (distinguished from my
usual state how?), blindness, changes in blood pressure, changes in body
temperature, changes in heart rate, chills, confusion, constipation, cough, dizziness,
fainting, feeling like you are not breathing even though you are (again? this one again?), fever, flushing,
headache, hives, irregular heartbeat, itching, jaw tightness, migraine, muscle
stiffness, nausea or vomiting that doesn't go away, numbness, rapid weight gain,
rash, redness, seizures, severe muscle pain or weakness, shortness of breath, sore
throat, swelling of the face (oh good, I've been wanting to try out my Violet Beauregarde impression), throat tightness, tingling, trouble swallowing, trouble
talking, uncontrolled movements of limbs or eyes, vomiting, yellowing of skin
or eyes, and/or -- now wait for it -- “any other side effects or symptoms.”
Really? Are you kidding me?
Short of my head falling off, what other side effects or symptoms could there
possibly be that haven’t already been identified? And for that matter, those of
you reading closely may notice there’s some significant overlap between the “call your doctor right away”
list and everything that came before. This leads to the obvious question: how,
pray tell, is one supposed to distinguish between, say, itching that warrants a call to the doctor and itching that's just par for the course?
Chemotherapy. Not for the faint of heart…
Friday, July 18, 2014
You Thought My Attitude Was Bad Before?
I find it interesting that the feedback I’ve gotten from this blog (from the
four or five people reading it, so I can't extrapolate too far) has divided
into two camps: there are those who think the posts reveal a healthy and positive
attitude toward the cancer experience; and then there are those who think the
exact opposite and, as nicely as they can, let me know that I’m not expressing
enough optimism and my expected survival would be improved if only I had a more
positive outlook.
Not to put too fine a point on it, but the latter group is starting to
annoy me.
I love you all dearly, but really? You really think my fundamental
problem is my attitude, rather than the malignant tumors that are currently taking over
my liver?
I’ve been thinking about this for a couple of days now, ever since I received
an email with a link to a survivor’s story on a website somewhere that
encouraged me to follow her lead and change my attitude to be more in line with
the survivor's. She was convinced she could be cancer, and did, so I could and should do the same. The question is, why do people think that the difference between cancer survival, and not, is a function of attitude?
After spending some time with the Google, I think I’ve identified the
answer: the entire freakin’ world thinks cancer survival, or not, is a function
of attitude. Which, when you think about it, basically boils down to a bunch of
people telling me that whether or not my cancer treatment is successful has
nothing to do with the type, state or progression of the cancer, nothing to do with
the doctors and care providers that are available to me, nothing to do with the treatment options I have to choose from,
it’s all about my attitude. If I choose to be appropriately positive and
“fight,” then my cancer will wither away and die; but if I choose otherwise, then I
will.
But why do so many people believe this? Personally, I blame Lance
Armstrong.
Let's think about Lance for a second. We all know Lance Armstrong had, and survived,
testicular cancer. So which explanation do you credit for his survival?
Option 1 – Lance had a fighter’s attitude and was committed to
surviving, so he did.
Option 2 – Cancer aside, Lance was in incredible health. His body was
in such amazing shape, not only could he actually complete in the grueling
competition that is the Tour de France, but he was able to win in multiple
times (and yeah, he cheated, but cheating was the difference between coming in first or coming in the top ten, not the difference between finishing the race or not). Moreover, having
won the Tour de France numerous times, Lance was -- what’s the word I’m looking
for? oh yeah... -- rich. Being rich gave Lance a vast range of alternatives for
his cancer treatment. He could see any doctor he wanted and opt for whatever
treatment he thought best. There were no constraints on his health care
options. Altogether then, because he was in amazing shape to begin with and had access to
the best care possible, Lance survived.
What boggles my mind is that Option 1 seems to be the answer
that most people choose. And as crazy as that seems to me, in truth I suppose I understand. Anyone (myself, perhaps,
excepted) can have a good attitude, but very few will ever be in the kind of shape and
have the kind of money and options that Lance had. Why wouldn’t someone prefer to identify
the difference between life and death as the resource they have access to (attitude) rather
than the ones they don’t (athleticism and money)?
But in many ways, Lance is just a particularly illustrative example of
a much broader problem with how cancer is all too frequently discussed and presented.
Let’s assume for the moment that people with cancer a) either survive or die,
and b) either have positive attitudes or negative attitudes. Reality is no
doubt more complicated, but for purposes here we can ignore the complications. So with these two binary variables, we get a matrix for cancer patients that looks
something like this…
Or, for those who don’t read matrices, we wind up with four groups of patients:
Group A – People who survived cancer and had a positive attitude
Group B – People who survived cancer, but had a negative attitude
Group C – People who did not survive cancer, but had a positive
attitude
Group D - People who did not survive cancer and had a negative
attitude
But here’s the thing: the only group anyone wants to talk about are the
folks in Group A. Look at the survivor pages on the various treatment center
webpages, and all you'll read about are people from Group A since those people survived and have positive, affective stories to tell. Moreover, the people in Group C can be presented as members of Group A, at least until the moment it becomes clear they aren't, actually, going to survive long term.
The consequences of all the attention on Group A are two-fold: first, everyone forgets that there are also people in Groups B, C and D; and second, without those counterexamples, it becomes all too easy to think that they key to survival is a positive attitude.
But those other groups do exist. I’m growing tired of this subject, so I won’t bother running through
all of them -- utilizing instead the classic dodge from a course in formal logic: “the remainder
of the proof is left as an exercise for the reader” -- but I will say that it’s extraordinarily
easy to find representatives from Group C.
Just Google three words together -- obituary,
cancer, and fighter -- and then weep for
...Eleni Vavas, a cardiologist who died at 37 from a rare stomach cancer.
...Ty Campbell, nicknamed the “Little Fighter,” who died of a rare brain cancer at the age of 5.
...Julia Wolf, a devoted mother who died of skin cancer at the age of 30.
...Talia Castellano, the adorable young girl who posted makeup tutorials to YouTube while she was being treated for her cancer, who died of neuroblastoma at age 13.
...and thousands more.
...Ty Campbell, nicknamed the “Little Fighter,” who died of a rare brain cancer at the age of 5.
...Julia Wolf, a devoted mother who died of skin cancer at the age of 30.
...Talia Castellano, the adorable young girl who posted makeup tutorials to YouTube while she was being treated for her cancer, who died of neuroblastoma at age 13.
...and thousands more.
I find it hard to believe anyone could look at how these people lived out their lives and say attitude has anything to do with survival.
I know everyone means well. I know everyone just wants the best for me.
But please, please, please try to remember that cancer is an indiscriminate
killer. Cancer kills people who are convinced they’re going to get better, and
it kills people who are convinced they’re going to die; at the same time, people who are
convinced they’re going to survive do, and people who are convinced they’re
going to die don’t. There is no rhyme or reason, and attitude is, at best, an extremely small factor in a much larger constellation of forces.
My attitude isn’t going to determine the outcome of my cancer. My
cancer and its response to the treatment will do that.
And by the way: if you really think my problem is that I need to have a
more positive attitude, just be aware that telling me so is likely not going to
have the desired effect. You won't get a positive outlook. What you'll get is a blog post like this one.
Thursday, July 17, 2014
There Is at Least One Good Thing About Cancer
Who knew, but there is one (very) good thing about cancer: it's extraordinarily useful for restoring one's faith in humanity.
When you have cancer people quickly begin to go out of their way to demonstrate how great they can be. At least that's been my experience. For example:
Food deliveries started a day or so after I got out of the hospital, and two weeks before my chemotherapy infusions start a co-worker has already created a web page soliciting ongoing deliveries to carry me through the first round of treatments. Unbelievable (to me anyway) numbers of people have signed up. And the one complaint about the schedule? There aren't enough opportunities for people to bring me food.
I've already mentioned all the people who visited me in the hospital, which was completely great, but now I've got folks offering to accompany me to my chemotherapy infusion appointments. How amazing is that? I have co-workers who want to take time off work, give me a ride to Group Health, and then sit in a little cubicle (or whatever it turns out to me) with me for hours while I'm filled with toxic chemicals and, presumably, grow increasingly miserable. There may even be vomiting. How nice does someone have to be to choose to spend their time like this?
Then there's the wanna be taxi drivers. Even though I live three blocks from Group Health, that particular organization won't let me leave from most appointments without someone else to escort me. I've had exactly no difficulty finding people who are willing to leave work and/or change the ways they get to work in order to provide me with the required escort.
As I mentioned earlier, all this cancer stuff came about in the midst of my S2BXS's and my divorce. And yet I've received cards and emails and texts from my S2BXS's family and friends -- people who likely thought they'd never have to interact with me again -- offering sympathy and assistance. It's incredibly nice of all these folks to look past the weirdness and reach out.
And how great is it to have your colleagues step up and cover for all your work while you're stuck in the hospital? Or to use their connections to get you access to facilities and appointments that you wouldn't otherwise have? Or to spend their time searching for treatment options and sources of support you might find helpful? Or to share their own cancer experiences so I have a little better idea of what you're in for? Or, for that matter, to do your grocery shopping or come over and do your laundry?
Granted, if given the choice I'd certainly opt to continue to be a misanthropic cancer-free nob. But if I have to have the cancer, being the beneficiary of so much kindness isn't the world's worst trade off.
And to everyone who's been so kind, thank you.
Update:
I knew I was going to forget something important. I forgot about the liver donor line up. Before I even had my surgery, Sib4 found an academic paper written by some doctors in Croatia describing how they used live donor liver transplant to cure a woman who's colon cancer had metastasized to her liver. Shortly, pretty much all my relatives were calling to let me know I could have their livers. A pretty nice, though sadly futile, gesture. Apparently, American oncologists aren't impressed with the treatments Croatia considers cutting edge. No live donor liver transplants here.
When you have cancer people quickly begin to go out of their way to demonstrate how great they can be. At least that's been my experience. For example:
Food deliveries started a day or so after I got out of the hospital, and two weeks before my chemotherapy infusions start a co-worker has already created a web page soliciting ongoing deliveries to carry me through the first round of treatments. Unbelievable (to me anyway) numbers of people have signed up. And the one complaint about the schedule? There aren't enough opportunities for people to bring me food.
I've already mentioned all the people who visited me in the hospital, which was completely great, but now I've got folks offering to accompany me to my chemotherapy infusion appointments. How amazing is that? I have co-workers who want to take time off work, give me a ride to Group Health, and then sit in a little cubicle (or whatever it turns out to me) with me for hours while I'm filled with toxic chemicals and, presumably, grow increasingly miserable. There may even be vomiting. How nice does someone have to be to choose to spend their time like this?
Then there's the wanna be taxi drivers. Even though I live three blocks from Group Health, that particular organization won't let me leave from most appointments without someone else to escort me. I've had exactly no difficulty finding people who are willing to leave work and/or change the ways they get to work in order to provide me with the required escort.
As I mentioned earlier, all this cancer stuff came about in the midst of my S2BXS's and my divorce. And yet I've received cards and emails and texts from my S2BXS's family and friends -- people who likely thought they'd never have to interact with me again -- offering sympathy and assistance. It's incredibly nice of all these folks to look past the weirdness and reach out.
And how great is it to have your colleagues step up and cover for all your work while you're stuck in the hospital? Or to use their connections to get you access to facilities and appointments that you wouldn't otherwise have? Or to spend their time searching for treatment options and sources of support you might find helpful? Or to share their own cancer experiences so I have a little better idea of what you're in for? Or, for that matter, to do your grocery shopping or come over and do your laundry?
Granted, if given the choice I'd certainly opt to continue to be a misanthropic cancer-free nob. But if I have to have the cancer, being the beneficiary of so much kindness isn't the world's worst trade off.
And to everyone who's been so kind, thank you.
Update:
I knew I was going to forget something important. I forgot about the liver donor line up. Before I even had my surgery, Sib4 found an academic paper written by some doctors in Croatia describing how they used live donor liver transplant to cure a woman who's colon cancer had metastasized to her liver. Shortly, pretty much all my relatives were calling to let me know I could have their livers. A pretty nice, though sadly futile, gesture. Apparently, American oncologists aren't impressed with the treatments Croatia considers cutting edge. No live donor liver transplants here.
Wednesday, July 16, 2014
By the Way, We're Now Caught Up
So at this point I've pretty much covered everything that happened -- well, the parts that I thought were worth writing about, at least -- from the time I entered the urgent care facility until now. The next major event will be the installation of a chest port to facilitate the chemotherapy infusions, but that's still a week away.
So at this point, the pace of my updates may slow as my treatment shifts from the sprint through surgery to the marathon of chemotherapy, the infusions for which will be scheduled to happen every other week.
Or maybe I'll just keep venting. Venting is good, and the cancer experience certainly provide plenty of things to vent about...
So at this point, the pace of my updates may slow as my treatment shifts from the sprint through surgery to the marathon of chemotherapy, the infusions for which will be scheduled to happen every other week.
Or maybe I'll just keep venting. Venting is good, and the cancer experience certainly provide plenty of things to vent about...
Lies, Damn Lies, and Statistics
I was a political science major in the late 1980s. No one knew it at the time, but this was the last days of the Cold War so there were a lot of classes -- a lot of classes -- focused on the various aspects of US-Soviet relations. In one such class I heard a story (possibly apocryphal) that has stuck with me:
The prof claimed that back in the day the Soviet government had used two different methods to drive the production of nails in the Soviet Union. When they rewarded nail production by count, the Soviet citizens got lots and lots and lots of little tiny nails. But when the government switched the production metric to weight, the tiny nails disappeared and the citizens got lots of big, giant spikes instead.
The purpose of the story was to illustrate the benefits of the market economy over a communist/socialist economy. But looking back now, I think the prof actually sold the story short. It's not about capitalist versus communist, it's about the power of metrics. I've now spent nearly twenty years in a career that involves working with significant numbers of operational metrics, and based on that experience I've learned two rules:
First, metrics have power. Counting, and establishing a system of rewards or punishments based on the selected counts, will drive behavior, no matter how intelligent -- or stupid -- the identified metrics may be.
Second, it's hard to develop a metric that can't be subverted.
Right or wrong, healthcare is now a metric driven endeavor, and has been for a very long time. As a result, and consistent with my rules, you don't have to hang out with healthcare providers for long to hear lots of stories about efforts to subvert the metrics. My favorite (weird word, but...) example of this was a story (again, possibly apocryphal) I heard of surgeons wheeling dying patients out of the operating room and into the hallway when a surgery went sideways as, apparently, whether the patient died in the operating room had significant impact on the metrics applied to the surgeon. Do I know it happened? No. Do I believe it could, or probably did? Absolutely.
I was thinking a lot about this after my visit with the SCCA. In cancer care, one of the primary metrics for evaluating everything is the five year survival rate. It doesn't take long Googling cancer to find examples survival curves like the one I inserted above. In that example, the conclusion we're all supposed to jump to is that the organization or provider or protocol represented by the green line is providing better care than that of the yellow.
Maybe, but providing better care is just one way to get to that result. The other way is to limit the number of truly unhealthy patients the green line takes on. If I'm the green line, and I can figure out a way to send the sickest patients to whatever the yellow line represents, I'll get the same result.* And frankly, it's the easier approach. I don't have to do anything different than anybody else is doing, I just have to figure out a way to keep the healthier patient with me (like, perhaps, by offering large, luxurious waiting rooms with stunning views of Lake Union -- just sayin'...).
I could, of course, be wrong. It could be that the possible impact I might have on the SCCA survival curve never once entered into anyone's calculation of whether I should be taken on as a patient. It could be that there were lots of other reasons focused on my best interests that drove the decisions that were made. It's certainly possible.
But the thing about me is I'm a cynical person. Moreover, my forty-six years on this planet have taught me that my problem is rarely that I'm too cynical; more frequently, it's that I haven't been cynical enough.
This, more than anything, has me wondering if that two-year survival median isn't going to be something of a stretch goal for me.
Damn statistics.
* Oddly enough, it was Oncologist #2 that inadvertently reminded me of this. In explaining to Sib4 why the Sloan-Kettering trial was less promising than the results suggested, he pointed out that the folks in the trial had to be healthy enough, and wealthy enough, to travel to New York and establish a life there while they underwent treatment. Thus, he argued, at least some portion of the positive results had to be credited to selection bias.
The prof claimed that back in the day the Soviet government had used two different methods to drive the production of nails in the Soviet Union. When they rewarded nail production by count, the Soviet citizens got lots and lots and lots of little tiny nails. But when the government switched the production metric to weight, the tiny nails disappeared and the citizens got lots of big, giant spikes instead.
The purpose of the story was to illustrate the benefits of the market economy over a communist/socialist economy. But looking back now, I think the prof actually sold the story short. It's not about capitalist versus communist, it's about the power of metrics. I've now spent nearly twenty years in a career that involves working with significant numbers of operational metrics, and based on that experience I've learned two rules:
First, metrics have power. Counting, and establishing a system of rewards or punishments based on the selected counts, will drive behavior, no matter how intelligent -- or stupid -- the identified metrics may be.
Second, it's hard to develop a metric that can't be subverted.
Right or wrong, healthcare is now a metric driven endeavor, and has been for a very long time. As a result, and consistent with my rules, you don't have to hang out with healthcare providers for long to hear lots of stories about efforts to subvert the metrics. My favorite (weird word, but...) example of this was a story (again, possibly apocryphal) I heard of surgeons wheeling dying patients out of the operating room and into the hallway when a surgery went sideways as, apparently, whether the patient died in the operating room had significant impact on the metrics applied to the surgeon. Do I know it happened? No. Do I believe it could, or probably did? Absolutely.
I was thinking a lot about this after my visit with the SCCA. In cancer care, one of the primary metrics for evaluating everything is the five year survival rate. It doesn't take long Googling cancer to find examples survival curves like the one I inserted above. In that example, the conclusion we're all supposed to jump to is that the organization or provider or protocol represented by the green line is providing better care than that of the yellow.
Maybe, but providing better care is just one way to get to that result. The other way is to limit the number of truly unhealthy patients the green line takes on. If I'm the green line, and I can figure out a way to send the sickest patients to whatever the yellow line represents, I'll get the same result.* And frankly, it's the easier approach. I don't have to do anything different than anybody else is doing, I just have to figure out a way to keep the healthier patient with me (like, perhaps, by offering large, luxurious waiting rooms with stunning views of Lake Union -- just sayin'...).
I could, of course, be wrong. It could be that the possible impact I might have on the SCCA survival curve never once entered into anyone's calculation of whether I should be taken on as a patient. It could be that there were lots of other reasons focused on my best interests that drove the decisions that were made. It's certainly possible.
But the thing about me is I'm a cynical person. Moreover, my forty-six years on this planet have taught me that my problem is rarely that I'm too cynical; more frequently, it's that I haven't been cynical enough.
This, more than anything, has me wondering if that two-year survival median isn't going to be something of a stretch goal for me.
Damn statistics.
* Oddly enough, it was Oncologist #2 that inadvertently reminded me of this. In explaining to Sib4 why the Sloan-Kettering trial was less promising than the results suggested, he pointed out that the folks in the trial had to be healthy enough, and wealthy enough, to travel to New York and establish a life there while they underwent treatment. Thus, he argued, at least some portion of the positive results had to be credited to selection bias.
I Don't Suppose I Could Have a Third Opinion
In retrospect, I was a moron. It was probably unreasonable to to think that when the oncologist tells you that there's not a whole lot that can be done, that they don't know precisely what they're talking about. But a) I've spent a long time supporting health care research and I believe in science, and b) if some doctor told you it was a coin toss as to whether you made it another two years, wouldn't you want to ask someone else? So it was time to explore what the Seattle Cancer Care Alliance's science-based treatment (at least that's how it's presented) might be able to offer.
Ultimately, the answer was, nothing. But we should probably back up.
When it came time to see Oncologist #2 at the SCCA, I elected to take Sib4 as my secondary listener in place of my S2BXS. Sib4 had spent the intervening weeks collecting numerous academic papers talking about possible cures for metastatic colon cancer, and I was frankly losing track. There was a liver transplant in Croatia, some heat-based thing happening in Germany, and, at least slightly closer to home, some promising clinical trial happening at Sloan-Kettering. Sib4 was convinced that one of these options would cure me, but I couldn't keep the details straight long enough to remember what questions she wanted me to ask. So I figured I'd bring her to the appointment so she could ask the oncologist herself.*
Checking in at SCCA was a far cry from Group Health. Where Group Health had a small waiting room with no one in it, the waiting room just for GI cancers at SCCA occupied the complete side of the building (with an amazing view of Lake Union) and was full of people. This was a cancer machine, and at least for the time in the waiting room that seemed promising.
Not so much. SCCA may be a cancer machine, but it turned out to be a machine that had little to offer me. Oncologist #2 instead confirmed that the treatment proposed by Oncologist #1 was the only treatment available. There were no other options at this stage of the treatment, though if I responded positively to phase one of the treatment there might be a clinical trial or other possibilities that might come into play. However, since the treatment SCCA could offer in the first phase wouldn't differ than what Group Health could offer, there was no way the financial gurus at Group Health would authorize treatment at SCCA. They'd been down that road before, and it wasn't worth the energy to fight the battle as they'd certainly lose. Oncologist #2 could agree to be available for future consults with Oncologist #1 as major milestones in my treatment were reached (or not), but that was the best SCCA could do for me.
He obviously didn't put it quite this way, and he, no doubt, would object, but the conclusion I drew from the conversation with Oncologist #2 was basically, "Yup, you're fucked."
I've spent most of my career working in support of science. It strikes me as a little sad that science didn't seem to be all that interested in returning the favor.
* The worst part of the appointment was when Sib4 got her opportunity to ask her questions. She went study by study and listened to Oncologist #2 explain in each case why what she found wouldn't, or couldn't, apply to me. By her nature, Sib4 is an optimistic person who I'm pretty sure was convinced that somewhere in all her papers she'd found the miracle cure. For my sake (obviously) and hers, I wish she hadn't had to be so thoroughly disappointed.
Ultimately, the answer was, nothing. But we should probably back up.
When it came time to see Oncologist #2 at the SCCA, I elected to take Sib4 as my secondary listener in place of my S2BXS. Sib4 had spent the intervening weeks collecting numerous academic papers talking about possible cures for metastatic colon cancer, and I was frankly losing track. There was a liver transplant in Croatia, some heat-based thing happening in Germany, and, at least slightly closer to home, some promising clinical trial happening at Sloan-Kettering. Sib4 was convinced that one of these options would cure me, but I couldn't keep the details straight long enough to remember what questions she wanted me to ask. So I figured I'd bring her to the appointment so she could ask the oncologist herself.*
Checking in at SCCA was a far cry from Group Health. Where Group Health had a small waiting room with no one in it, the waiting room just for GI cancers at SCCA occupied the complete side of the building (with an amazing view of Lake Union) and was full of people. This was a cancer machine, and at least for the time in the waiting room that seemed promising.
Not so much. SCCA may be a cancer machine, but it turned out to be a machine that had little to offer me. Oncologist #2 instead confirmed that the treatment proposed by Oncologist #1 was the only treatment available. There were no other options at this stage of the treatment, though if I responded positively to phase one of the treatment there might be a clinical trial or other possibilities that might come into play. However, since the treatment SCCA could offer in the first phase wouldn't differ than what Group Health could offer, there was no way the financial gurus at Group Health would authorize treatment at SCCA. They'd been down that road before, and it wasn't worth the energy to fight the battle as they'd certainly lose. Oncologist #2 could agree to be available for future consults with Oncologist #1 as major milestones in my treatment were reached (or not), but that was the best SCCA could do for me.
He obviously didn't put it quite this way, and he, no doubt, would object, but the conclusion I drew from the conversation with Oncologist #2 was basically, "Yup, you're fucked."
I've spent most of my career working in support of science. It strikes me as a little sad that science didn't seem to be all that interested in returning the favor.
* The worst part of the appointment was when Sib4 got her opportunity to ask her questions. She went study by study and listened to Oncologist #2 explain in each case why what she found wouldn't, or couldn't, apply to me. By her nature, Sib4 is an optimistic person who I'm pretty sure was convinced that somewhere in all her papers she'd found the miracle cure. For my sake (obviously) and hers, I wish she hadn't had to be so thoroughly disappointed.
Subscribe to:
Posts (Atom)